“Your waistline is not only about weight. It is about risk.” – Wellness Kraft
Introduction
Most men do not wake up worried about metabolic syndrome. They wake up concerned about work, money, time, and stress. The belly grows in the background like a slow app update you never approved.
It usually starts innocently. Your jeans fit tighter. You loosen the belt one notch. You tell yourself you will fix it next month. Then next month becomes next year. Meanwhile, you are still “functioning,” so your brain files it under “not urgent.”
Metabolic syndrome is why thinking can be expensive.
Because metabolic syndrome is not one disease, it is a pattern. It is your body waving five small flags, and if at least three are up, the long-term risk climbs: type 2 diabetes, heart disease, stroke, and other complications.
Here is the uncomfortable truth: you can look “not that overweight” and still have metabolic risk if your fat is concentrated around the belly and your blood markers are drifting in the wrong direction. Some men with “normal” body weight still carry metabolic syndrome. It is not about appearance. It is about what is happening inside.
If you have been telling yourself, “I will start later,” read this as if it were later.
What Metabolic Syndrome Actually Means
Metabolic syndrome is a cluster of risk factors that tend to travel together. Think of it as a warning dashboard, not a diagnosis of “you are doomed.”
The standard components are:
- Higher waist circumference (abdominal obesity)
- Higher triglycerides
- Lower HDL (“good” cholesterol)
- Higher blood pressure
- Higher fasting blood sugar (or related blood sugar abnormality)
You do not need all five to be at risk. The problem is when several stack together. That stack strongly increases your chance of developing diabetes and cardiovascular disease over time.
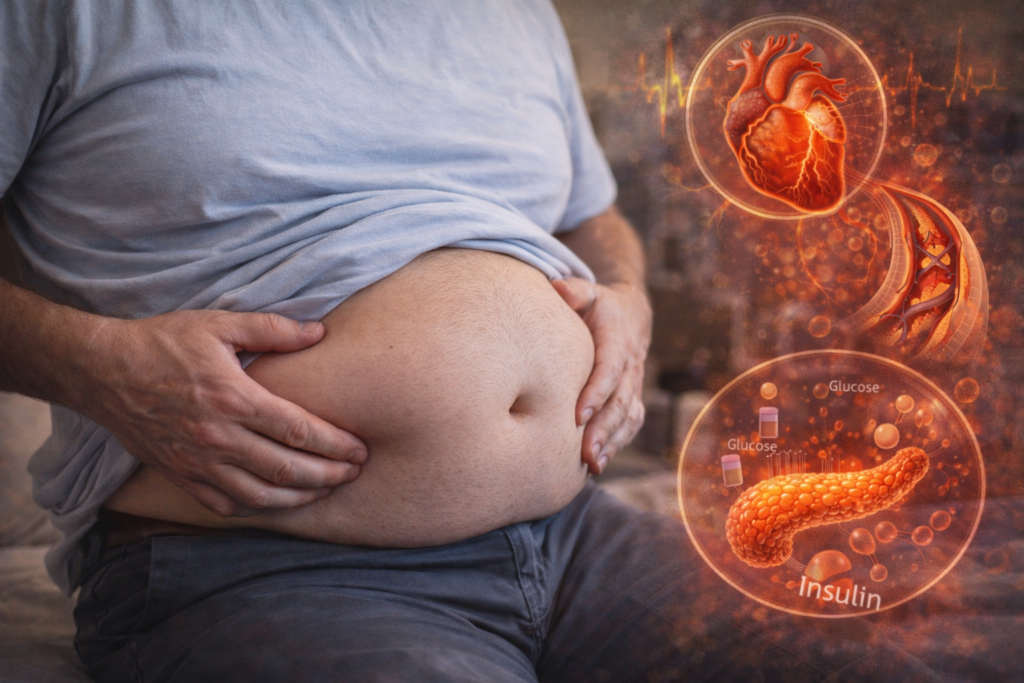
Now here is the key: belly fat is not passive storage. Deep belly fat behaves more like an active organ. It releases signals that can worsen insulin resistance and inflammation. That is why the belly is often the first visible sign of an internal shift.
Why Belly Fat Is Different From “Just Fat”
There are two broad types of fat in the abdomen.
One sits closer to the skin. That is the softer layer you can pinch.
The other is visceral fat, deeper, around organs. This deep fat is strongly linked to metabolic risk.
Visceral fat is not “lazy fat.” It isn’t quiet. It can influence how your liver handles fat and sugar, how your muscles respond to insulin, and how much inflammatory signaling is happening in the background.
That is why some men gain ten pounds and feel fine, while another man gains ten pounds and suddenly has high blood pressure, borderline sugar, and awful fatigue—the location and type of fat matters.
If you are thinking, “Okay, but how do I know what kind of belly fat I have?”
You do not need a scan to start. Your waist measurement is a simple and powerful clue.
A Story Most Men Recognize
Brian is 38. He does not consider himself unhealthy. He does not smoke. He drinks on weekends. He walks sometimes. He eats “okay” most days. He is busy and tired, like everyone.
His belly has been growing slowly for years. Not dramatic. Just enough that he stopped tucking in shirts. He jokes about it. His friends joke about it. Nobody treats it like a health issue.
Then one day, he is in a pharmacy and checks his blood pressure for fun. The number is high enough that he checks again. Still high. He laughs it off, but it stays in his head.
A month later, he does routine labs for work insurance. His fasting blood sugar is higher than expected. His triglycerides are up. His HDL is low. The clinician says a phrase Brian has heard before but never absorbed: “You are trending toward metabolic syndrome.”
Brian’s first reaction is annoyance. He thinks, “I am not that overweight.”
His second reaction is fear. He thinks, “What if diabetes is coming and I do not see it?”
What changed him was not panic. It was clarity. He realized the belly was not only about weight. It was information. His body had been sending signals, and he had been treating them like background noise.
This is the most common story about metabolic syndrome. No drama. Just a man who is “fine” until the numbers prove he is not as fine as he thought.
The Early Signs Men Commonly Ignore
Metabolic syndrome does not always announce itself loudly. It often shows up as subtle lifestyle friction.
You may notice:
You get sleepy after meals more than before.
You crave sugar or snacks late at night.
Your energy feels flat even after sleep.
Your waist size grows while your weight seems “stable.”
Your blood pressure readings are creeping upward.
You think more about brain fog than you used to.
You feel short of breath faster during regular activity.
None of these proves metabolic syndrome, but they are reasons to check your dashboard.
A useful self-question is this:
“Am I getting older, or am I getting metabolically worse?”
Age happens. Metabolic decline can be slowed and often reversed, especially early.
The Simple Checklist That Matters
If you want one practical action today, it is this: measure your waist and check your numbers.
Waist matters because it tracks abdominal fat better than body weight alone.
Numbers matter because metabolic syndrome is detected through standard clinical measures: waist circumference, blood pressure, blood lipids (triglycerides and HDL), and fasting glucose.
You do not have to become a medical expert. You have to stop operating blind.
If you have not checked these in the last year, that is your starting point.
Why Metabolic Syndrome Leads to Bigger Problems
Metabolic syndrome increases risk because it represents a system under strain.
When blood sugar is elevated, the body is struggling to regulate insulin.
When triglycerides are high and HDL is low, the lipid system is off-balance.
When blood pressure is high, your blood vessels are under chronic stress.
When abdominal fat is high, inflammatory and metabolic signals often worsen.
This combination accelerates atherosclerosis (plaque buildup), worsens insulin resistance, and raises long-term risk for heart attacks and strokes.
This is why men should treat metabolic syndrome as a prevention moment, not a label to fear.
How to Fix It Without Living Like a Monk
The most effective approach is not “diet harder.” It is “change the system that created the belly.”
Here is what actually works when done consistently.
1) Build a meal pattern your body can trust
Most metabolic chaos comes from unpredictable eating: long gaps, late overeating, constant snacking, and high sugar swings.
Instead of chasing a perfect diet, start with a stable structure:
Eat enough protein in the day so you are not hunting for food at night.
Add fiber so your blood sugar rises more slowly.
Reduce ultra-processed snacks that spike appetite and cravings.
A practical way to eat without obsession is to make each meal look like this:
A solid protein base, a significant portion of vegetables or lentils/beans, and a controlled portion of starch, with healthy fats not “free-poured.”
If you want one behavior that gives fast results, it is cutting liquid calories and sweet drinks. They are the easiest calories to overconsume and the least satisfying.
2) Walk after meals
Post-meal walking is one of the most underrated metabolic tools. It helps glucose management without needing a gym session. Even ten to fifteen minutes after meals can help your body handle sugar better.
This is where men win because it is simple and repeatable. You do not need motivation. You need a routine.
3) Strength training is not optional if you want long-term change
Muscle is a metabolic ally. It improves insulin sensitivity, supports healthy glucose storage, and makes weight loss easier to sustain.
If you hate gyms, do fundamental home strength: squats, push-ups, rows, lunges, and core work. The goal is consistency, not perfection.
4) Fix sleep because sleep shapes appetite and insulin
Poor sleep increases hunger hormones, increases cravings, worsens stress tolerance, and can worsen insulin resistance. If your sleep is broken, your discipline will always feel harder than it should.
If you snore loudly, wake up tired, or feel sleepy during the day, consider sleep apnea screening. Sleep apnea is closely tied to metabolic risk in many men.
5) Reduce alcohol frequency, not only quantity
Many men focus on “how much,” but the more important question is “how often.”
Alcohol can worsen sleep quality, increase belly fat over time through excess calories, and often triggers late-night eating. You do not need to quit forever. You need to stop pretending it has no metabolic cost.
6) Stress is not an excuse, but it is a factor
Chronic stress pushes cortisol patterns, worsens sleep, and drives cravings. The goal is not to eliminate stress. The goal is to stop using food and screens as the only coping tools.
Even one daily habit that lowers your nervous system can help: a walk outside, a short breathing routine, or a strict “phone off” time at night.
What to Ask Your Doctor
If you want a clean conversation with your clinician, ask for a metabolic risk check that includes:
Waist measurement or discussion of abdominal obesity
Blood pressure
Fasting glucose or HbA1c
Lipid panel (triglycerides and HDL included)
Then ask the most helpful question:
“Which three changes would move my numbers the fastest in the next 12 weeks?”
That keeps the plan practical.
Key Takeaways
- Belly fat, intense abdominal fat, is closely linked to metabolic risk.
- Metabolic syndrome is a cluster of risk factors that raises the chance of diabetes and heart disease when several occur together.
- You can have metabolic syndrome even if you are not “visibly obese.”
- The most effective improvements usually come from consistent sleep, post-meal walking, strength training, and simpler eating patterns.
- Measuring waist and checking blood pressure, fasting glucose, and lipids is the smartest starting point.
Research Insight
Major health organizations describe metabolic syndrome as a group of conditions that together increase the risk of heart disease, stroke, and type 2 diabetes, and they outline diagnosis using common measures like waist circumference, triglycerides, HDL cholesterol, blood pressure, and fasting blood glucose. NHLBI, NIH+2NHLBI, NIH+2
Public health research using US population data has found that metabolic syndrome is associated with higher mortality risk, including in adults who are not obese by BMI, reinforcing that “normal weight” does not always mean “low risk.” CDC
Reviews and public health summaries also note that metabolic syndrome increases risk of cardiovascular disease and type 2 diabetes, and emphasize early identification and lifestyle intervention. CDC+1
https://www.nhlbi.nih.gov/health/metabolic-syndrome
https://www.nhlbi.nih.gov/health/metabolic-syndrome/diagnosis
https://www.cdc.gov/pcd/issues/2020/20_0020.htm
https://www.cdc.gov/pcd/issues/2022/21_0231.htm
https://www.ahajournals.org/doi/10.1161/circulationaha.105.169405
FAQs
1) Can I have metabolic syndrome if my weight is not “that high”?
Yes. Weight alone does not tell the whole story. If fat is concentrated around the abdomen and your blood pressure, triglycerides, HDL, and glucose are drifting in the wrong direction, risk can be high even if BMI looks “normal.” This is why waist measurement and lab markers are so important.
2) Why is belly fat worse than fat in other areas?
Deep abdominal fat around organs tends to be more metabolically active. It can influence insulin resistance and inflammation and is strongly associated with higher cardiometabolic risk. That is why two men of the same weight can have very different health profiles depending on where fat is stored.
3) What is the fastest lifestyle change that improves metabolic markers?
Most men see the quickest early improvements from a combination of post-meal walking, reduced sugary drinks, and ultra-processed snacking, and better sleep. The “best” change is the one you can repeat daily, because consistency beats intensity for metabolic health.
4) If I lose weight, will metabolic syndrome go away?
Often, metabolic markers improve significantly with weight loss, especially when abdominal fat reduces. Still, the best results usually come from combining weight change with strength training, better sleep, and improved food quality. Some men can improve markers even before significant weight loss by improving activity and meal patterns.
5) What tests should I check to know where I stand?
Common screening includes waist measurement, blood pressure, fasting glucose or HbA1c, and a lipid panel that includes triglycerides and HDL. These are standard, accessible tests that can quickly show whether you are trending toward metabolic syndrome.
Concluding Thoughts
Belly fat is not a character flaw. It is a signal. And metabolic syndrome is not a life sentence. It is a warning light that turns on early enough for you to do something about it.
The men who win in the long term are not the men who go extreme for two weeks. They are the men who build simple routines that run even on stressful days: walking after meals, lifting a few times a week, sleeping as it matters, and eating in a way that keeps blood sugar stable.
If you want a clean starting line, make it this: measure your waist, check your numbers, then give yourself 12 weeks of consistent changes. Your future heart will not clap, but it will keep beating, and that is the point.




Join the conversation